Mental health service overview
Boab Health Services is committed to delivering high-quality, evidence-based, stepped-care mental health services for people in the Kimberley.
This page is designed to help inform health professionals about our treatment options, eligibility criteria and referral process for our various mental health services. Visit Our Service – Mental Health for a general overview of our mental health services and programs.
Service eligibility criteria – overview
To be eligible for our mental health service, an individual must be experiencing barriers to accessing the Medicare Benefits Schedule (MBS) system (e.g. low income, job insecurity, social isolation etc.). Individuals cannot access an MBS mental health (Better Access) service and Boab Health mental health service concurrently. Individual program eligibility is described below under each service type.
The type of intervention we offer an individual is based on the severity of their presentation. The severity of presentation is determined from the information included in your referral and our intake assessment of the individual.
Priority clients
Priority is given to individuals who are at disproportionate and inequitable risk of poor health outcomes including:
- Aboriginal and Torres Strait Islander people
- Culturally and linguistically diverse people (CALD)
- People of diverse sexuality and/or gender (LGBTIQ+)
- People with histories of suicidal ideation or self-harm behaviours.
Exclusion criteria
We do not provide the following services:
- long-term therapy
- support for clients in an acute phase of illness
- immediate or urgent support
- treatment for complex post-traumatic stress disorder, personality disorders, dementia, delirium, or intellectual disability.
Service locations
Our Mental Health Team visits Balgo, Bidyadanga, Billiluna, Broome, Dampier Peninsula communities, Derby, Fitzroy Crossing, Halls Creek, Kalumburu, Kununurra, Mulan, Warmun, Wyndham and some communities in the Fitzroy Valley. Some services are location specific. Please see
View our locations and frequency of service map for more details.
Intervention types
We aim to support individuals to enhance their self-management skills to improve their mental health outcomes. We offer a range of short-to-medium term supports, including psychological counselling, psycho-education, self-help strategies, group programs and referrals to other supports and resources, including online (Mindspot GP) and telephone counselling options.
Treatment plan pathway
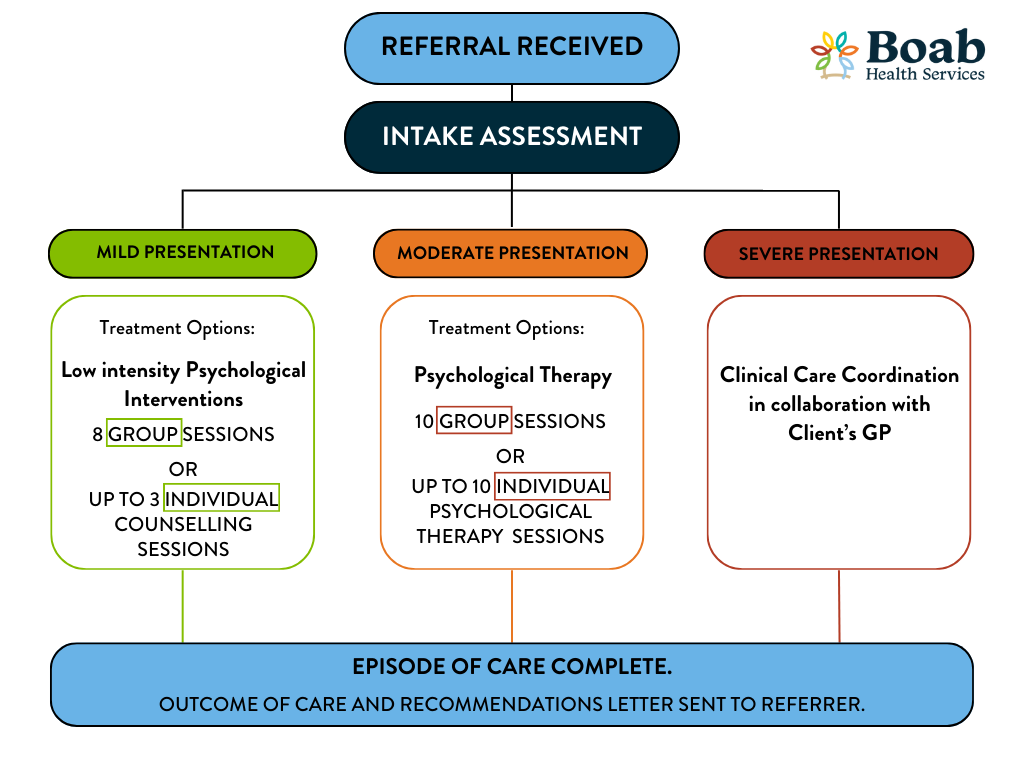
Eligibility criteria for specific interventions
We offer short-term individual psychological support and counselling for people experiencing mild-to-moderate mental health concerns. We facilitate individual counselling either via PORTS online or telephone support or face-to-face counselling with one of our Mental Health Professionals depending on the severity of the presentation.
The number of face-to-face individual counselling sessions an individual will be eligible to receive will be determined during the initial assessment. This is typically up to three individual sessions for mild presentations or up to 10 individual sessions for moderate presentations. See our treatment options diagram above for more details.
Our group programs and courses differ from group therapy. During these programs, we aim to empower individual’s with knowledge, tools, and practical skills to help improve their mental wellbeing. Confidentiality is assured during group programs. Individuals are not asked to disclose personal circumstances in our group programs.
Evidence suggests group programs can be just as effective and sometimes more effective than individual counselling. Group programs can help people feel less alone and provide an opportunity for induvial to hear from others experiencing similar issues. For a list of our current programs, click here.
Our Clinical Care Coordination (CCC) program supports individuals with severe mental illness that impacts their daily functioning.
We support GPs with the case management of people experiencing severe mental illness by providing care coordination and supports, including counselling. CCC is nurse-led support that involves working collaboratively with the GP to perform:
- initial and ongoing assessment,
- treatment planning,
- liaising/linking with other agencies,
- assisting when there is deterioration of symptoms,
- liaison and psychoeducation with family and carers.
We require a GP referral to access this service.
Our child mental health service provides developmentally appropriate counselling to children aged 0-12 years and their parents or carers. This service aims to assist children and families overcome common mental health concerns.
Our child counselling service utilises evidence-based child-specific modalities and interventions such as play therapy, child-centred parenting support, cognitive behavioural therapy, and mindfulness strategies to allow children to communicate and express feelings and experiences in a safe and supportive environment.
This service is currently available in our Broome and Kununurra offices and may be available in other locations via Telehealth. Contact us for more information.
We require parent or guardian consent and a GP/Paediatrician, Midwife or Child Health Nurse, or CAMHS professional referral to access this service.
Our youth mental health service supports youth aged 12 – 25 years who are experiencing difficulties with their mental wellbeing, have a diagnosed mental health condition (mild to moderate) or are experiencing suicidal thoughts or self-harm .
Our services may include individual counselling, family therapy, group programs, linking young people to other resources and working with other services to foster youth engagement and emotional wellbeing health promotion.
We involve parents and/or carers, and family as appropriate (depending on the age and/or consent of the young person) and require a GP/Psychiatrist/Paediatrician or CAMHS professional referral to access this service.
Our Kununurra-based youth counselling and support program provides clinical mental health services and family support for young people aged 11 to 18 years of age who are currently enrolled at a school in Kununurra.
This service supports young people (and their family/carers) experiencing, or at risk of developing, complex or severe mental health issues who would benefit from intensive support.
We provide specialist mental health counselling, community support, care coordination and tailored therapeutic groups. This is a flexible service to provide an engaging and positive experience for young people.
We require parent or guardian consent and a GP referral to access this service.
The A Better Life (ABLe) program aims to improve the independence, participation and long-term wellbeing of people living in Wyndham who are affected by mental health issues, including drug and alcohol misuse and/or gambling.
This program aims to building resilience and supports participants to sustainably manage the impacts of their mental health issues. This program is open to people living in Wyndham, who are aged 16 to 65 years.
If you would like to no more about this program. contact our Youth & Community Support Coordinator (ABLe Program) on 0437 589 842 or email reception@boabhealth.com.au.
We do not require referrals to our ABLe program in Wyndham.
This program supports culturally safe, community-driven strengths and resilience initiatives to promote mental health and wellbeing for people living in the remote communities of Balgo, Billiluna and Mulan. Our mental health community development officer is based in Balgo Aboriginal community for two weeks each month.
Contact our Balgo Community Development Officer on 0438 899 297 or email reception@boabhealth.com.au for more information about this program. Please note we do not require a GP referral to access the community development program in Balgo.
Referral form and pathways
We require a referral for the majority of our programs and services. You can find our mental health referral form here. Contact us if you would like a Microsoft Word version of this referral form to upload to your patient management system. Please ensure the referral includes:
- The specific service you require
- The client’s most recent contact details including a telephone number, email address, postal or street address
- K10, K5 or SDQ (for children – contact us for this form) objective measure as indicated on the referral form
Please complete all fields on the referral form or send a comprehensive MHCP. This ensures we are able to process the referral, triage and contact the client in a prompt and timely manner.
Who do we accept referrals from?
We accept referrals from GPs, psychiatrists, paediatricians, remote area nurses, midwives and maternal and child health nurses, or from Kimberley Mental Health and Drug Services (KMHDS) professionals (including CAMHS).
What about self-referrals?
Self-referrals, referrals from other agencies and referrals from friends or family will also be considered where there is difficulty obtaining a GP referral, particularly in remote communities. Where the referral is not from a GP, psychiatrist or paediatrician, our team will seek to obtain GP endorsement of the proposed treatment plan following our initial assessment.
Where do I send the referral?
Email: reception@boabhealth.com.au
Fax: (08) 9192 7999
Via MMEx Secure Messaging: ‘Boab Health – Counselling’
Do I need to include a Mental Health Care Plan (MHCP) with the referral?
No, an MHCP is not essential. However, it is helpful for our clinicians to have a Mental Health Care Plan (MHCP) or a Chronic Disease Management Plan (formerly EPC plan) included with the referral. This provides our clinicians with a holistic view of the individual’s health and wellbeing and the flexibility to treat the individual under MBS if their presentation is more suited to the Medicare funding criteria.
Referral process
- Once we receive the referral, we triage the referral and send a confirmation letter to the referring GP.
- Our Triage and Assessment officer will arrange an appointment with the individual to undertake the initial assessment and develop a treatment plan. The treatment plan will typically recommend individual counselling, phone or online support via Mindspot GP, referral to a group program or an alternative service, or a combination of these, as appropriate.
- We will inform the referrer of the treatment plan. Where counselling is indicated, both the referrer and client will be informed of the wait time to engage with a counsellor. Interim support options will be discussed with the individual as appropriate.
- The Boab Mental Health clinician allocated to deliver the treatment plan will update the referrer periodically with the individual’s progress.
Prompts to consider when referring
Sometimes we find that clients are not therapy-ready. Inappropriate referrals can demotivate the client and unduly extend our waitlist. To assist you in determining if a referral to our service is appropriate, our Triage and Assessment team have created the prompts below.
It is essential the client understands and supports a referral for counselling.
We will attempt to contact a client up to three times by telephone. If we do not hear back from the clients, we will send a letter requesting contact. If we do not hear from the client within two weeks from sending the letter, we will close the referral.
Anglicare WA offers relationship counselling in Broome and Kununurra.
As we are a free service with funding limitations our wait times can sometimes be up to three months. Other services may be more appropriate for immediate or situational concerns or crises, including telephone counselling via PORTS, employee assistance programs or private practitioners. See below for more information on how to refer to these services.
You may also be able to link your client with other services in your local area that can assist with practical day-to-day matters.
PORTS is a free telephone or online counselling service. Options include four one-hour telephone counselling sessions, or an 8-week online CBT based program (with telephone support).
PORTS contact clients very quickly (within a few days) and the service is individualised to meet the client’s needs. PORTS is ideal for a short-term intervention, for example in cases of situational crises and mild mental health problems. PORTS specialise in dealing with anxiety, stress, depression and substance use.
If this service would be suitable for your client, complete our standard referral form indicating the client would like a PORTS referral.
A number of private psychologists / counsellors are available in Broome. These private services can be accessed through a GP Mental Health Care Plan. The fee gap ranges from no charge (bulk billed) to up to $100 per session, depending on the practitioner. Private practitioners generally have a much shorter wait time for treatment and may have speciality / interest areas that might be better suited to your client’s presentation. Also, private psychologists are better placed to assist clients with medico-legal issues and cognitive disorders or neuro-psychology concerns.
Please contact our Triage and Assessment Officer if you would like information about private practitioners available in the Kimberley.
Some clients may have access to an EAP through their employer that provide employee counselling (often also available for family members). Your client may not have considered accessing their EAP.
Headspace is a multidisciplinary service for young people aged 12 to 25 years. They often have a shorter wait time for assistance.
A referral to the Kimberley Mental Health and Drug Service (KMHDS) Community Alcohol and Drug Services team for counselling is required if the presenting issue is problematic alcohol and / or other drug (AOD) use. Once the AOD problem has resolved as the primary concern, our mental health clinicians can provide counselling to address other ongoing issues. For other AOD service providers, see the end of this page.
How do we treat DNA’s?
For initial appointments, we typically allow two DNAs (without client making contact) before closing the referral.
Accreditation

Funding
Our programs are primarily funded by WAPHA and we operate within the scope of the WAPHA program guidelines.
Our staff
Our team is made up of highly skilled mental health professionals with expertise and experience in supporting a variety of mental health conditions. Our clinical mental health professionals are tertiary qualified and highly experienced in counselling.
Other local support services
Kimberley wide supports:
WACHS’s Kimberley Mental Health and Drug Service
Broome tel: (08) 9194 2640
Kununurra tel: (08) 9166 4350
WACHS’s Child and Adolescent Mental Health Service
Broome tel: (08) 9194 2640
Kununurra tel: (08) 9166 4350
Alcohol and other drug service providers in the Kimberley
Milliya Rumurra Aboriginal Corporation (Broome and Kununurra) Tel: (08) 9192 1699
Cyrenian House (Broome)
Ngnowar Aerwah Rehabilitation Centre – (08) 9161 2109 (Wyndham)
Other support services in Broome:
